One of the most perplexing questions about SARS-CoV-2, the virus that causes COVID-19, is how it spreads so rapidly between people. Scientists know it can be transmitted by droplets from a sneeze or cough. But can it spread through aerosols, the smaller particles we give off when we exhale or speak? How long do infectious particles linger in the air? How far can they travel?
These questions dominated an Aug. 26-27 workshop of the Environmental Health Matters Initiative, (EHMI), organized by the National Academies of Science, Engineering, and Medicine (NASEM) and co-sponsored by NIEHS. Experts in aerosol science, virology, infectious disease, and epidemiology presented what is known about airborne transmission of SARS-CoV-2 to more than 14,000 viewers worldwide. See the workshop webpage for session recordings.
 Individual behaviors like wearing masks are one factor in determining a person’s environmental risk, according to John Volckens, Ph.D., from Colorado State University.
Individual behaviors like wearing masks are one factor in determining a person’s environmental risk, according to John Volckens, Ph.D., from Colorado State University.To inform response policies, organizers wanted to synthesize current knowledge and highlight data gaps. “We are discussing a virus that none of us knew existed a year ago,” said Jay Butler, M.D., deputy director for infectious diseases at the Centers for Disease Control and Prevention.
“Airborne transmission of SARS-CoV-2 is plausible,” he cautioned. “Our approaches need to be data-based and not dogma-based.”
Infection trifecta
A virus, no matter how new and mysterious, needs an environment that brings it together with a host in order to spread. Each component forms one corner of the epidemiologic triangle, which scientists use to understand infectious diseases.
The importance of the environment became more evident this year, said Thomas Burke, Ph.D., of Johns Hopkins University. “COVID changed everything and forced us to take a hard look at how we define environment,” he said.
Besides air, water, and land — the usual aspects of the natural environment — built structures such as housing, workplaces, schools, transportation, and infrastructure must also be reckoned with.
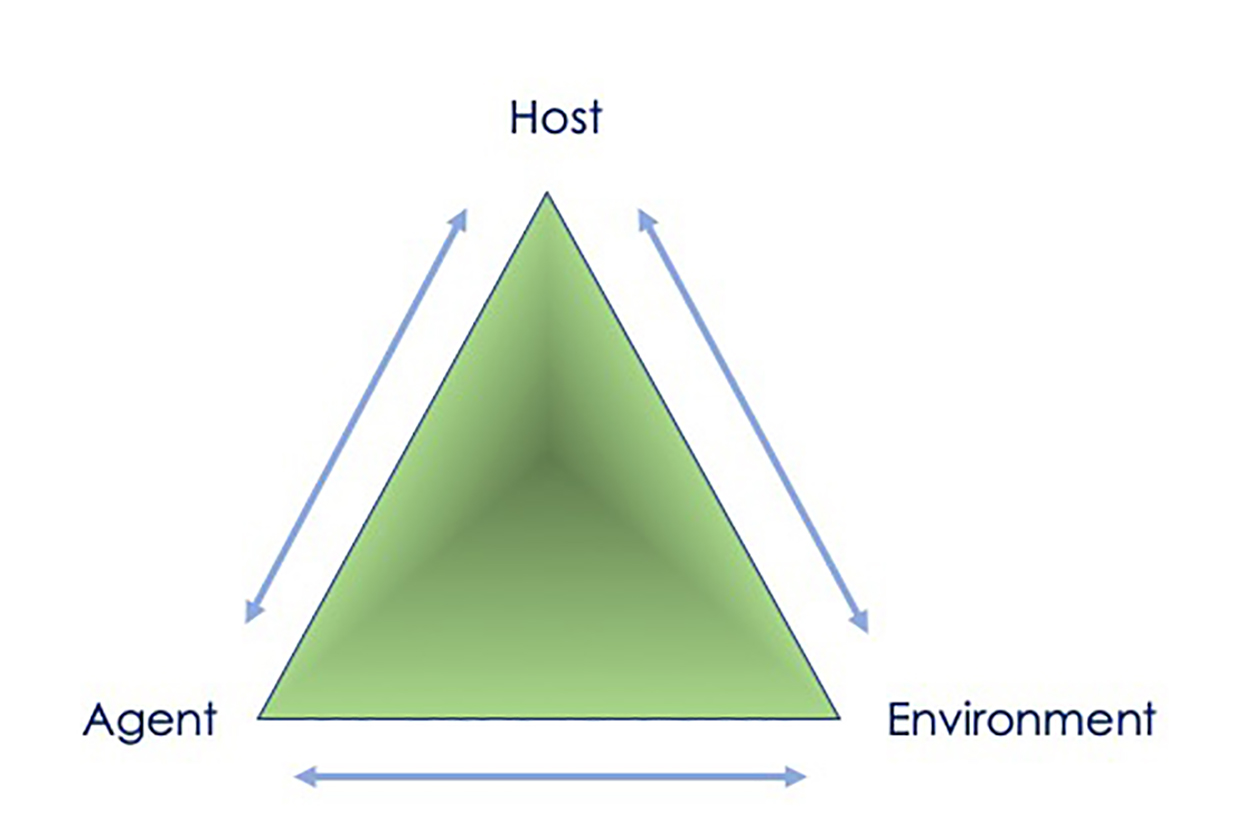 The epidemiologic triangle portrays interactions among agent, or SARS-CoV-2; host, or humans; and environment. They are connected by a vector — humans, in this case. (Image courtesy of NIEHS)
The epidemiologic triangle portrays interactions among agent, or SARS-CoV-2; host, or humans; and environment. They are connected by a vector — humans, in this case. (Image courtesy of NIEHS)Fixing the environment
Disparities in the built environment likely contribute to the racial health disparities in COVID-19, according to several speakers. “Where you work and live impacts exposure and possible transmission,” said Shelly Miller, Ph.D., of the University of Colorado at Boulder.
In a study of immigrant housing in Denver, she found people living in crowded and poorly ventilated quarters. Carbon dioxide and particulate matter levels increased with the number of people in a home.
Ventilation, air cleaning, and ultraviolet radiation can reduce indoor aerosols. But Miller cautioned against do-it-yourself approaches. “You do not want to just spray chemicals to disinfect the air … because that will generate this indoor chemistry that will cause health issues,” she said. “We need to stick to tried-and-true methods.”
The evidence mounts
Experts shared current evidence on SARS-CoV-2 airborne transmission, including:
- Asymptomatic individuals spread the virus.
- Breathing and talking can produce 100 to 1,000 times more aerosols than droplets.
- Aerosols remain suspended in the air for hours and can move many meters from the source. Especially indoors, a six-foot separation may not be enough to avoid exposure.
- Superspreading events, which lead to an unusually high number of new infections, suggest the virus can spread through the air.
- Transmission is greatly reduced outdoors compared with indoors.
- Laboratory animals release virus-laden aerosols that can infect susceptible individuals.
“It is pretty clear … that aerosols represent an important transmission pathway for SARS-CoV-2,” said former NIEHS grantee Kim Prather, Ph.D., of Scripps Institution of Oceanography and the University of California San Diego.
“It is also clear that definitions of droplet and aerosol, which are traditionally differentiated at a size of 5 microns, should be updated to reflect that a droplet this size can linger in the air for half an hour or more,” she said afterwards.
Workshop participants stressed that the line between droplets and aerosols is better drawn at 100 microns, rather than the 5-micron cutoff used by aerosol scientists and others. “Size determines whether transmission is by inhalation or contact, how long the particles remain in the air, the distance they travel, and severity of disease,” Prather said.
Addressing behavior
The complexity of SARS-CoV-2 calls for layering behavioral strategies like hand hygiene, social distancing, and wearing masks, rather than a single intervention.
“Behavior is a social science that needs to be woven into our research as we focus on prevention,” said long-time NIEHS grantee and planning committee member John Volckens, Ph.D., of Colorado State University.
(Marla Broadfoot, Ph.D., is a contract writer for the NIEHS Office of Communications and Public Liaison.)