Two NIEHS researchers found that the external genitalia of male and female mice begin exhibiting different cell populations early in fetal development. They made the discovery by examining the cells that give rise to the male penis and female clitoris. The research was published in the Proceedings of the National Academy of Sciences.
 While the early fetal mouse cells of the penis and clitoris look the same under a microscope, Amato saw differences in their gene production. (Photo courtesy of Steve McCaw / NIEHS)
While the early fetal mouse cells of the penis and clitoris look the same under a microscope, Amato saw differences in their gene production. (Photo courtesy of Steve McCaw / NIEHS)The NIEHS scientists responsible for the work, NIEHS postdoctoral fellow Ciro Amato, Ph.D., and his mentor Humphrey Yao, Ph.D., head of the NIEHS Reproductive Developmental Biology Group, said identifying different cell populations within the developing fetus may help scientists find ways to understand the causes of some external genitalia birth defects that occur in human males and females.
One of these common birth defects in males is called hypospadias, and it occurs when the opening of the urethra, or the tube that carries urine out of the body, does not form at the tip of the penis. Instead, the opening may happen anywhere along the shaft of the penis, even at the base of the organ near the scrotum. According to U.S. birth defects data, the incidence of hypospadias is 1 in every 120 newborn boys.
'Surgical correction of hypospadias is difficult because it is soft tissue, so when it scars, the penis can become deformed, and the patient will have to go back for multiple surgeries,' Amato said. 'If we have a better understanding of what the cell populations are doing, we may be able to develop better treatment strategies.'
Single-cell sequencing
Yao said that at the start of the project, he and Amato knew there were cells that produced androgen receptors in the penis and estrogen receptors in the clitoris. They just did not know which cells and how similar or different they were. He credited Amato for using a new approach to address this question called single-cell sequencing technology. The technique sequenced the mRNA — the RNA strand that is complementary to one of the DNA strands of a gene — from individual cells of mouse external genitalia.
 “Our goal was to identify the different cell populations that exist in the fetal external genitalia of the mouse,” Yao said. (Photo courtesy of Steve McCaw / NIEHS)
“Our goal was to identify the different cell populations that exist in the fetal external genitalia of the mouse,” Yao said. (Photo courtesy of Steve McCaw / NIEHS)'The method allowed us to basically perform a census to figure out how many different cell populations were present,' Yao said.
After they found several subpopulations of cells and determined their characteristics, Amato and Yao were able to identity every cell within the penis, grouping them based on their similarities and differences. The method generated a lot of data. With the help of the NIEHS Integrated Bioinformatics Support Group and other colleagues at the institute, Amato used his biostatistical skills and knowledge of computer programming to write all the code he needed to analyze the data.
Environmental impact
Yao and his research group study how reproductive organs, such as gonads, reproductive tract, and external genitalia, form during the development of an embryo, known as embryogenesis. They also examine whether this process is susceptible to in utero exposure to endocrine disruptors in the environment. Endocrine disruptors are chemicals that mimic or interfere with the body’s hormones. He said many chemicals induce hypospadias in experimental animal models.
'Hypospadias is a common birth defect, but there hasn’t been a lot of research on it, because it is a private matter,' Amato said. 'Our paper opens up the field and provides a way for future researchers to study the condition.'
Citations:
Amato CM, Yao HH-C. 2021. Developmental and sexual dimorphic atlas of the prenatal mouse external genitalia at the single-cell level. Proc Natl Acad Sci U S A 118(25):e2103856118.
Mai CT, Isenburg J, Langlois PH, Alverson CJ, Gilboa SM, Rickard R, Canfield MA, Anjohrin SB, Lupo PJ, Jackson DR, Stallings EB, Scheuerle AE, Kirby RS; National Birth Defects Prevention Network. 2015. Population-based birth defects data in the United States, 2008 to 2012: Presentation of state-specific data and descriptive brief on variability of prevalence. Birth Defects Res A Clin Mol Teratol 103(11):972–993.
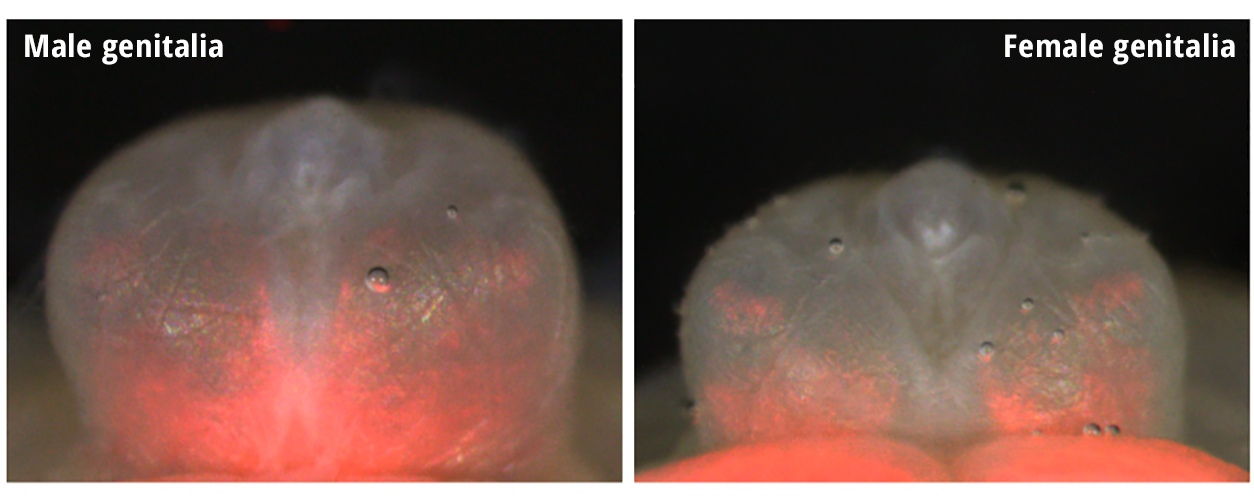
The micrograph of male (left) and female (right) genitalia from mouse embryos shows a specific group of cells, stained red, that occurs in both sexes. (Image courtesy of Ciro Amato and Humphrey Yao)