Today on World Asthma Day, the National Institutes of Health (NIH) stands with patients, families, advocates, researchers, and health care professionals to raise awareness about this common chronic respiratory disease, the people it affects, and the biomedical research that improves its prevention and treatment.
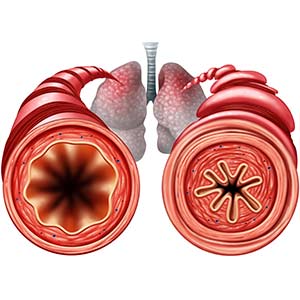
Asthma is a chronic lung disease that causes periods of wheezing, chest tightness, shortness of breath, and coughing. It is a major contributing factor to missed time from school and work, with severe attacks requiring emergency room visits and hospitalizations. Asthma attacks can sometimes be fatal.
 According to CDC, common asthma triggers include tobacco smoke, dust mites, outdoor air pollution, pets, and mold, among others.
According to CDC, common asthma triggers include tobacco smoke, dust mites, outdoor air pollution, pets, and mold, among others.This year, we recognize that the coronavirus disease 2019 (COVID-19) pandemic is creating concern and uncertainty for many people around the globe, including those with asthma. The disease can affect the nose, throat, and lungs, cause an asthma attack, and possibly lead to pneumonia and acute respiratory disease.
According to the Centers for Disease Control and Prevention (CDC), people with asthma should continue their current asthma medications and discuss any concerns with their health care provider. Researchers at NIH and elsewhere are working to learn more about COVID-19 and to develop specific treatments and vaccines.
Three NIH institutes support and conduct studies on asthma — the National Institute of Environmental Health Sciences (NIEHS); the National Heart, Lung, and Blood Institute (NHLBI); and the National Institute of Allergy and Infectious Diseases (NIAID). Institute scientists and grantees made several important advances in understanding, treating, and managing asthma in 2019. These findings and other highlights are featured in the five topic areas below.
- Relationship between asthma and COVID-19.
- Populations at risk of developing asthma.
- Potential new treatments.
- Genes involved in asthma.
- Asthma management.
Relationship between asthma and COVID-19
NIAID is initiating a home-based study to assess the incidence of infection with SARS-CoV-2, the virus that causes COVID-19, in children, their caregivers, and siblings. A key objective of this observational study will be to determine whether infection rates or immune responses to SARS-CoV-2 infection differ in children who have asthma or other allergic conditions compared with those who have not been diagnosed with or treated for these conditions.
NIAID also is starting an observational study in patients hospitalized for COVID-19 to understand whether specific characteristics of the immune response influence or reflect the severity of infection. This study may help determine whether underlying diseases, such as asthma, influence the body’s response to SARS-CoV-2 infection.
Populations at risk of developing asthma
Children
NIH scientists are making progress in understanding the underlying factors that contribute to the development of asthma in U.S. children. This year, an international collaboration led by NIEHS scientists reported that the presence of newly discovered novel epigenetic markers — or chemical tags that attach to DNA — may indicate a newborn’s risk of developing asthma.
The data were generated by the Pregnancy and Childhood Epigenetics Consortium and may help researchers find asthma biomarkers, or molecular indicators of asthma, and identify at birth which children will eventually develop the condition.
At NHLBI, researchers discovered a link between childhood asthma flare ups and changes in the lung microbiome, which refers to communities of bacteria and other microorganisms that are normally present in the lung and usually do not cause symptoms. The scientists determined that children with mild to moderate asthma who experienced early signs of an upcoming asthma flare up tended to have higher levels of certain types of disease-causing bacteria in their lungs. The study could lead to a precision medicine approach for treating mild to moderate childhood asthma by altering the number and types of bacteria in a child’s airways.
Ongoing NIAID-funded clinical studies focus on interventions to prevent asthma development in children at high risk of developing the condition. One team of researchers studied a large group of children who were hospitalized as infants with bronchiolitis, a common early-life lung infection usually caused by a virus. The scientists found that recurrent wheezing by age 3 is at least three times more likely to occur in children whose bronchiolitis was associated with a rhinovirus C infection and who also had early signs of allergy to foods or inhaled allergens.
African Americans and people of African ancestry
Another group that bears a disproportionate burden of asthma is African Americans. In an NHLBI-funded study that is the largest genome-wide association study of asthma in African ancestry populations to date, researchers identified two novel regions on a specific chromosome that may be linked to asthma risk. The scientists theorize that a better understanding of the genetic risk factors for asthma in African ancestry populations will lead to development of better therapeutic interventions.
Potential new treatments
Using a mouse model of asthma, NIEHS researchers reported a possible treatment for neutrophilic asthma, a particularly severe form that responds poorly to the standard asthma therapy of corticosteroids.
The orally available drug VTP-938 made it easier for the mice to breathe after they were exposed to house dust extracts. The results suggest that VTP-938 may be an innovative treatment for humans with this steroid-resistant form of asthma.
Genes involved in asthma
An NIAID-funded study sought to understand why some, but not all, colds lead to asthma attacks among children with asthma. The scientists obtained nasal washings from 106 children with severe asthma who experienced cold symptoms. Members of the research team compared samples from those who required corticosteroids after a cold-induced asthma attack and those who did not have an asthma attack following a cold.
The research team found that colds that led to an asthma attack caused changes in the production of six families of genes that are associated with maintaining the function of the outermost layer of tissue lining the respiratory tract and with the responses of immune cells in close contact with this layer.
Variations in two genes — the aryl hydrocarbon receptor nuclear translocator (ARNT) and the protein tyrosine phosphatase, nonreceptor type 22 (PTPN22) — are associated with immune-mediated diseases, such as asthma, in several ethnicities, according to NIEHS researchers and their collaborators.
Because ARNT and PTPN22 are sensitive to environmental factors, this study is the first to demonstrate across ethnicities the combined role of these genes and environmental changes in the development of immune-related conditions such as asthma.
Asthma management
The NHLBI National Asthma Education Prevention Program is coordinating the 2020 focused updates to the 2007 Asthma Management Guidelines. These guidelines are designed to improve the care of people living with asthma as well as help primary care providers and specialists make decisions about asthma management.
NHLBI released the updated focus areas of the guidelines for public comment, and the final recommendations for these areas are expected to be published later this year. They will address the priority topic areas listed below.
- Using inhaled medications when needed.
- A new type of inhaled medication called long-acting muscarinic antagonists.
- Treating allergies by exposure to low doses of allergens by mouth or with shots.
- Reducing indoor asthma triggers.
- A new procedure for asthma known as bronchial thermoplasty.
- A fractional exhaled nitric oxide test that may help in diagnosing or managing asthma.
Experts hope that these guidelines will help reduce the burden of asthma nationwide and improve the quality of life for those living with the condition.
NIEHS, NHLBI, and NIAID focus on specific areas of research, but all three have the common goal of developing improved strategies for asthma prevention, treatment, and management.
- NIEHS supports research to understand the effects of the environment on human health and is part of the National Institutes of Health.
- NHLBI is the global leader in conducting and supporting research in heart, lung, and blood diseases and sleep disorders that advances scientific knowledge, improves public health, and saves lives.
- NIAID conducts and supports research — at NIH, throughout the United States, and worldwide — to study the causes of infectious and immune-mediated diseases, and to develop better means of preventing, diagnosing, and treating these illnesses.
Citations:
Reese SE, Xu CJ, den Dekker HT, Lee MK, Sikdar S, Ruiz-Arenas C, Merid SK, Rezwan FI, Page CM, Ullemar V, Melton PE, Oh SS, Yang IV, Burrows K, Soderhall C, Jima DD, Gao L, Arathimos R, Kupers LK, Wielscher M, Rzehak P, Lahti J, Laprise C, Madore AM, Ward J, Bennett BD, Wang T, Bell DA; BIOS consortium, Vonk JM, Haberg SE, Zhao S, Karlsson R, Hollams E, Hu D, Richards AJ, Bergström A, Sharp GC, Felix JF, Bustamante M, Gruzieva O, Maguire RL, Gilliland F, Baiz N, Nohr EA, Corpeleijn E, Sebert S, Karmaus W, Grote V, Kajantie E, Magnus MC, Ortqvist AK, Eng C, Liu AH, Kull I, Jaddoe VWV, Sunyer J, Kere J, Hoyo C, Annesi-Maesano I, Arshad SH, Koletzko B, Brunekreef B, Binder EB, Raikkonen K, Reischl E, Holloway JW, Jarvelin MR, Snieder H, Kazmi N, Breton CV, Murphy SK, Pershagen G, Anto JM, Relton CL, Schwartz DA, Burchard EG, Huang RC, Nystad W, Almqvist C, Henderson AJ, Melen E, Duijts L, Koppelman GH, London SJ. 2019. Epigenome-wide meta-analysis of DNA methylation and childhood asthma. J Allergy Clin Immunol 143(6):2062–2074.
Zhou Y, Jackson D, Bacharier LB, Mauger D, Boushey H, Castro M, Durack J, Huang Y, Lemanske RF Jr, Storch GA, Weinstock GM, Wylie K, Covar R, Fitzpatrick AM, Phipatanakul W, Robison RG, Beigelman A. 2019. The upper-airway microbiota and loss of asthma control among asthmatic children. Nat Commun 10(1):5714.
Hasegawa K, Mansbach JM, Bochkov YA, Gern JE, Piedra PA, Bauer CS, Teach SJ, Wu S, Sullivan AF, Camargo CA Jr. 2019. Association of rhinovirus C bronchiolitis and immunoglobulin E sensitization during infancy with development of recurrent wheeze. JAMA Pediatr 173(6):544–552.
Daya M, Rafaels N, Brunetti TIM, Chavan S, Levin AM, Shetty A, Gignoux CR, Boorgula MP, Wojcik G, Campbell M, Vergara C, Torgerson DG, Ortega VE, Doumatey A, Johnston HR, Acevedo N, Araujo MI, Avila PC, Belbin G, Bleecker E, Bustamante C, Caraballo L, Cruz A, Dunston GM, Eng C, Faruque MU, Ferguson TS, Figueiredo C, Ford JG, Gan W, Gourraud PA, Hansel NN, Hernandez RD, Herrera-Paz EF, Jimenez S, Kenny EE, Knight-Madden J, Kumar R, Lange LA, Lange EM, Lizee A, Maul P, Maul T, Mayorga A, Meyers D, Nicolae DL, O’Connor TD, Oliveira RR, Olopade CO, Olopade O, Qin ZS, Rotimi C, Vince N, Watson H, Wilks RJ, Wilson JG, Salzberg S, Ober C, Burchard EG, Williams LK, Beaty TH, Taub MA, Ruczinski I, Mathias RA, Barnes KC; CAAPA. 2019. Association study in African-admixed populations across the Americas recapitulates asthma risk loci in non-African populations. Nat Commun 10(1):880.
Whitehead GS, Kang HS, Thomas SY, Medvedev A, Karcz TP, Izumi G, Nakano K, Makarov SS, Nakano H, Jetten AM, Cook DN. 2019. Therapeutic suppression of pulmonary neutrophilia and allergic airway hyperresponsiveness by a RORyt inverse agonist. JCI Insight 4(14): e125528.
Schuman SH, O’Hanlon TP, McGrath JA, Gruzdev A, Bektas A, Xu H, Garantziotis S, Zeldin DC, Miller FW. 2019. Transethnic associations among immune-mediated diseases and single-nucleotide polymorphisms of the aryl hydrocarbon response gene ARNT and the PTPN22 immune regulatory gene. J Autoimmun 102363.