The National Toxicology Program (NTP) concluded in a final report released March 4 that researchers found a moderate level of evidence that workplace exposure to chemotherapy drugs is associated with an increased risk of miscarriage and genetic toxicity.
Studies identified through a literature review also suggested that workplace exposures to these drugs have decreased over time, as institutions provide protective equipment and employees follow safe handling guidelines.
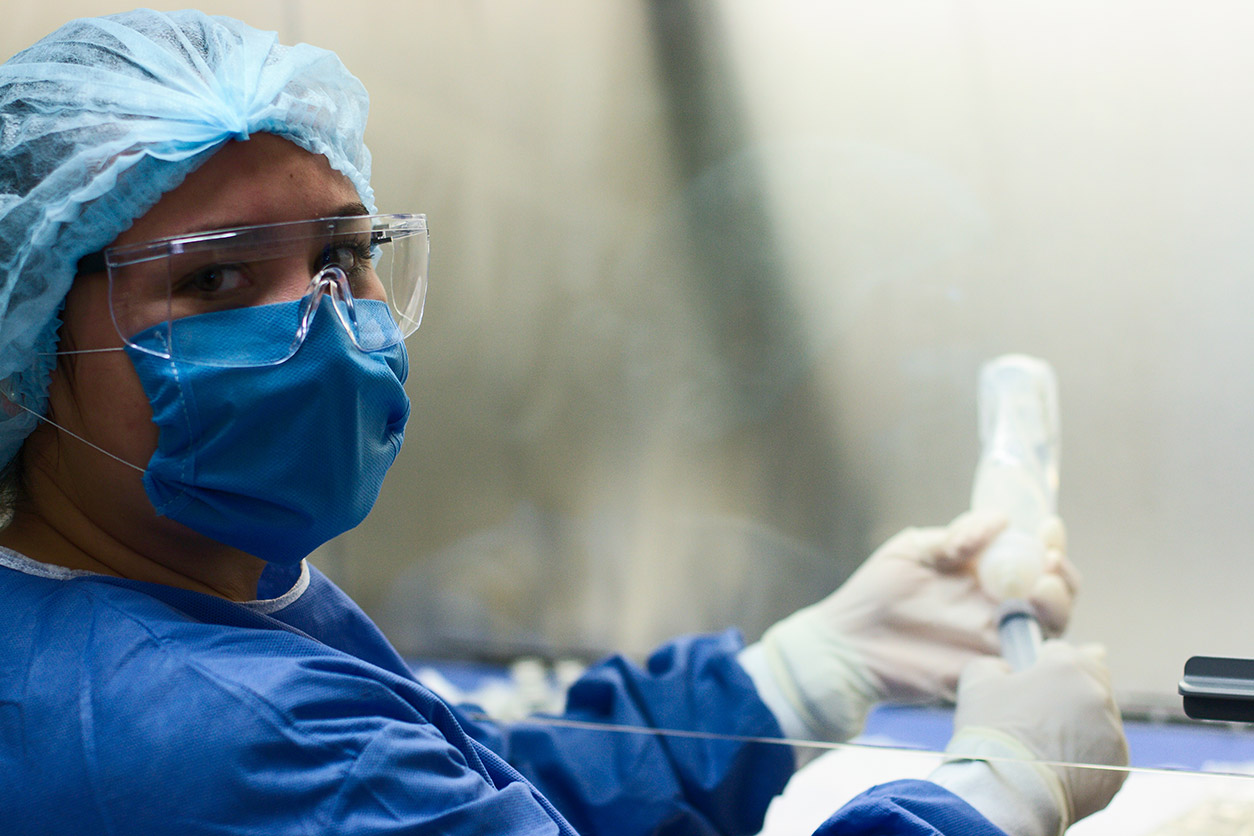 The new NTP monograph is based on studies of groups of workers, like pharmacists and oncology nurses, who prepare and administer chemotherapy drugs. (Image courtesy of Jose Eugenio Gomez Rodriguez under a CC BY-SA 3.0.)
The new NTP monograph is based on studies of groups of workers, like pharmacists and oncology nurses, who prepare and administer chemotherapy drugs. (Image courtesy of Jose Eugenio Gomez Rodriguez under a CC BY-SA 3.0.)“That decrease in exposure is good news,” said the lead scientist for the evaluation, Kembra Howdeshell, Ph.D., of the NTP Office of Health Assessment and Translation (OHAT).
“Chemotherapy drugs play an important role in treating cancer and autoimmune diseases,” she explained. “However, we know that treatment with chemotherapy can result in secondary cancers such as leukemia, suppression of the immune system, and other negative side effects. Furthermore, miscarriage and birth defects have been observed in many laboratory animal studies of the effects of exposure to these agents during pregnancy.”
Health effects
 Howdeshell, from NTP, led the project from conception to publication. (Photo courtesy of Steve McCaw)
Howdeshell, from NTP, led the project from conception to publication. (Photo courtesy of Steve McCaw)The NTP monograph on the “Systematic Review of Occupational Exposure to Cancer Chemotherapy Agents and Adverse Health Outcomes” is a follow-up to the 2013 NTP monograph on the effects of chemotherapy use during pregnancy, which focused on women who were pregnant while being treated for cancer. The new publication addresses potential adverse health effects in workers who administer these drugs or may otherwise be exposed to them at work.
NTP performed a comprehensive literature search that identified 110 epidemiological studies that assessed possible adverse health outcomes. The scientists also identified 171 studies that evaluated exposures. The conclusions were reviewed by agency partners and five outside experts.
Using a scale of high, moderate, low, and inadequate evidence, NTP reported a moderate level of evidence that workplace exposure to chemotherapy drugs is associated with an increased incidence of miscarriage.
The scientists also found a moderate level of evidence that workplace exposure to chemotherapy drugs is associated with genetic toxicity, or DNA damage. This damage may be corrected through cells’ repair mechanisms. However, if not corrected, such damage could result in mutations that may lead to cancer. Therefore, genetic toxicity is frequently monitored in workers exposed to chemotherapy drugs.
There was inadequate evidence for other adverse health outcomes, including cancer, due to the limited numbers of studies or to mixed results.
 Rooney contributed to the project through the conception and drafting of the protocol, and drafting of the report. (Photo courtesy of Steve McCaw)
Rooney contributed to the project through the conception and drafting of the protocol, and drafting of the report. (Photo courtesy of Steve McCaw)Reducing exposures
The researchers also found that as recently as 2016, chemotherapy drugs were detected in workers’ urine and blood samples, as well as in the work environment. Yet some studies suggested that workplace exposure levels are decreasing, due to increased awareness and use of safety procedures.
“Some of the greatest uncertainty in this evaluation is due to the lack of detailed information on exposure of health care workers to chemotherapy drugs,” said Andrew Rooney, Ph.D., OHAT acting director. “Medical surveillance programs will provide data critical to protecting these workers.” Such programs enroll health care workers for biomonitoring and environmental monitoring in the workplace.
Environmental monitoring provides information on potential exposures by testing for chemotherapy drugs on workplace surfaces and in air. Biomonitoring can confirm recent exposures through analysis of urine and blood samples of people working around the drugs.
Authors of the monograph also identified the need for further development and validation of other ways to document workplace exposure such as daily diaries that document drug-handling activities, personal protective equipment use, and possible exposures, such as from spills.
 Lawson (see sidebar) critically reviewed the protocol as well as the draft report and figures. (Photo courtesy of Tina Lawson)
Lawson (see sidebar) critically reviewed the protocol as well as the draft report and figures. (Photo courtesy of Tina Lawson)Most of the studies reviewed by NTP looked at medical care professionals, like pharmacists and oncology nurses, who prepare and administer these drugs. The study also looked at reports on other potentially exposed worker populations.
The authors emphasized the need for more health and exposure studies of hospital housekeeping personnel, veterinary clinic staff, and family and friends caring for cancer patients at home.
(Marla Broadfoot, Ph.D., is a contract writer for the NIEHS Office of Communications and Public Liaison.)









